Resources
Menopause FAQs
.
What is menopause?
Menopause (meno– relating to the menstrual cycle, –pause meaning stop) refers to the final menstrual period; technically, it is said to have occurred 12 consecutive months (one year) after the final period. This happens when the ovaries stop releasing eggs and levels of hormones (oestrogen, progesterone and testosterone) fall.
The vast majority of people affected by menopause identify as women, and the discourse around menopause tends to reflect this. However, menopause also happens to people of differing genders who were assigned female at birth (AFAB), including transmasculine, intersex and non-binary people.
Menopause is natural process, but can also occur as a result of surgery to remove the ovaries (called a bilateral oophorectomy), medical treatment (e.g., following radio- or chemotherapy), infection, autoimmune conditions (e.g., type 1 diabetes) and genetic causes (e.g., Turner syndrome).
The average age of menopause in the UK is 51 years of age. Menopause between the ages of 40 and 45 is called early menopause, and is estimated to affect approximately 12% of women in the UK. If it occurs below the age of 40 it is termed premature ovarian insufficiency (POI), or premature menopause; on a global scale, POI is believed to affect around 3.5% girls and women.
Although a cause for early menopause or POI is not always found, it can sometimes run in families. Some women may experience an early menopause as a result of having a hysterectomy (removal of the womb), even if they do not have their ovaries removed at the same time.
How is menopause diagnosed?
If you are over 45 years of age and are experiencing menopausal symptoms, together with a change in your menstrual cycle (your periods may have become irregular or more frequent, may be lighter or heavier), then no tests are needed to diagnose the menopause. If you are using contraception that stops your periods (e.g., the progestogen-only pill or a hormone containing coil such as the Mirena IUS) or have had a hysterectomy, then it would be a good idea to write down your symptoms, or record them using an electronic app, and discuss these with your GP.
If you are under 45 years of age and believe you are experiencing menopausal symptoms, you will need to have a blood test to measure the level of a hormone called follicle stimulating hormone (FSH). This blood test is often repeated 4-6 weeks later. If you are below the age of 40 you will require other tests to ensure you have the correct diagnosis.
What are the symptoms of menopause?
Pre-menopause, the hormones oestrogen and progesterone work together to release eggs from the ovaries and regulate your menstrual cycle. During the perimenopause, the levels of oestrogen and progesterone fluctuate widely and the imbalance in these hormones can lead to menopausal symptoms. Other symptoms are often a result of an overall low level of oestrogen in the body. Many different parts of the body can be affected, including the bones, joints, heart, brain, skin and vagina.
Over 80% of women will experience some menopausal symptoms, but the severity of these can vary hugely. Symptoms can start several years before the final period (during the perimenopause) and may continue for months to years after menopause (during postmenopause). Surgical menopause – which occurs following surgical removal of the ovaries – results in immediate menopause, with no transitional phase, and hormone levels drop significantly within hours; symptoms can arise suddenly and may be severe.
Hot flushes are one of the most common menopausal symptoms and affect around three out of four women. These are often felt as a sudden sensation of warmth which spreads throughout the body. They may be associated with sweating, dizziness, anxiety and feeling sick or light-headed. Hot flushes often come on suddenly, but certain things can also trigger them e.g., after drinking alcohol, coffee or eating spicy food, smoking cigarettes.
Other symptoms include: irregular or heavy periods, night sweats, joint pains, poor sleep (insomnia), heart palpitations, low mood (depression), anxiety, mood swings, poor memory, tiredness, headaches, vaginal dryness, hair and skin changes, urinary symptoms (needing to pass urine more frequently), painful sex, and low sexual desire (low libido).
The average length of time for women to experience symptoms is 7 years, but around 10% will experience symptoms for more than 15 years. In surgical menopause, without treatment, symptoms may be life-long.
Are there any long-term health problems associated with menopause?
After menopause, women have an increased risk of osteoporosis (thinning of the bones), heart disease and dementia. This is believed to be as a result of the falling levels of oestrogen, as this hormone protects our bones, heart and our brain.
Hormone replacement therapy (HRT) may help reduce these risks. For this reason, it is very important, if possible, for women who experience an early or premature menopause to take HRT until at least the age of 51.
There are also things you can do to help yourself to reduce your risk of long-term health problems after the menopause, including eating a well-balanced diet, exercising regularly and reducing stress (see below).
What can I do to help myself during menopause?
Stopping smoking, if this is relevant to you, is one of the best things you can do to reduce your symptoms and improve long term health. Consider seeking support/smoking-cessation therapy if you feel you will struggle to do this alone.
There is some evidence that women who follow a plant-based, fibre-rich, diet experience fewer menopausal symptoms. They also have lower rates of heart disease, diabetes and cancer. Even if you do not follow a fully plant-based diet, aim to focus your meals around fruits, vegetables, whole-grains, beans/legumes, nuts and seeds. Include foods rich in phyto-oestrogens (plant-based oestrogens) in your daily diet e.g., soya beans, chickpeas/hummus, and lentils. Minimise highly processed and refined foods, including sugar and junk food, and alcohol.
Some women find that spicy food, caffeinated drinks (coffee, tea and cola) and alcohol worsen their symptoms (especially hot flushes and night sweats). Alcohol and caffeine can also exacerbate psychological symptoms (e.g., anxiety and low mood) and can be detrimental to bone health, so aim to keep these to a minimum (or eliminate completely).
Ensuring you have adequate sleep (7-8 hours a night) is paramount, but menopausal symptoms (especially night sweats) can make this difficult. Make sure your bedroom is well-ventilated, wear light natural clothing e.g., cotton pyjamas, or sleep naked, and consider investing in a fan.
To minimise sleep disruption, switch off electronic devices at least one hour before bed and/or wear blue light blocking glasses in the evening. Aim to get up at approximately the same time each day and get outside in the morning daylight (whatever the weather) for at least 20 minutes. If this is not possible, try to have your breakfast/morning drink close to a window/in a naturally lit area. This will help to regulate your sleep cycle (and hormones).
Exercise is very important for physical and mental well-being, symptom reduction and bone, brain and heart health. Aim to move your body daily. If you are able to hike, run, or dance, for example, these are fantastic for improving bone density; if not, Pilates and yoga can provide similar benefits and are also important for developing strength and improving balance. Both cardiovascular exercise (activity that raises your heart rate for a sustained period of time) and weight-bearing exercise (that forces your body to work against gravity) and resistance exercises (activity that increases lean muscle mass, reduces body fat and increases strength – such as lifting weights) are equally important.
Stress reduction can have a hugely positively impact on menopausal symptoms. 5-10 minutes of mindfulness meditation and/or breathing exercises, for example, can be incredibly beneficial. Overall, be kind to yourself and aim to allow yourself at least 15-30 minutes a day to do something just for you e.g., reading a novel, listening to your favourite music/podcast, walking in nature.
Are there any supplements I should consider taking during menopause?
Everybody over the age of 50, regardless of dietary choices, should take a regular vitamin B12 supplement. Aim for 10 micrograms daily, or at least 2000 micrograms once a week. If you follow a vegetarian or vegan diet, then B12 supplementation is recommended regardless of age. Vitamin B12 is important for bone, heart and brain health and can reduce the risks of the long-term health concerns associated with menopause.
Vitamin D3 is important for everyone in the UK between the months of October and April. This is because we do not have enough sunlight in the northern hemisphere at this point in the year to make this vitamin (which is technically a hormone itself). Aim for 10 micrograms/ (400 IU) – 25 micrograms (1000 IU) daily. In spring/summer, try and get at least 20 minutes’ exposure to sun on your arms/legs/back (no sunscreen); if this is not possible, then continue to supplement. Vitamin D3 is particularly important for bone health, but also plays a part in oestrogen metabolism.
Iodine is important when it comes to hormonal, and bone, health and many people are deficient in this mineral (in many countries salt is iodised to guard against this, but this is not the case in the UK). Adults require 140 micrograms daily (do not exceed 0.5 milligrams a day and avoid kelp-based supplements).
An affordable and reliable supplement that contains vitamin B12, D3 and iodine is the VEG1 supplement from The Vegan Society (you do not, of course, need to be vegan to take this supplement).
Consider taking an algae-derived (sustainable) EPA/DHA omega-3 supplement (250 – 600 milligrams daily) or add 1 tablespoon of ground flaxseed and 6 walnut halves to your daily diet. Omega-3 fatty acids are essential for good heart and brain health. Igennus have developed a good quality omega-3 supplement, which is one I often recommend (although there are others out there).
Other supplements may be recommended on an individual basis, dependent on your symptoms and/or medical history.
Please note, I have no financial ties, and receive no commission, from either The Vegan Society or Igennus; I recommend their supplements based on personal, and clinical, experience alone.
What medical treatments are available to help with the symptoms of menopause?
If you experience mild menopausal symptoms these may improve with dietary and lifestyle changes alone, and medical treatment may not be required. However, if you experience difficult symptoms that are negatively impacting your quality of life, it would be worth seeking medical input for further advice and support (please do not suffer in silence – help is available!).
Hormone replacement therapy (HRT) is the most effective medical treatment for symptoms of the menopause, and also helps protect your brain, heart and bones. All HRT contains the hormone oestrogen and, for women who have not had a hysterectomy, a progestogen (a synthetic form of progesterone).
HRT is available as tablets, gel, spray or patches to be placed on the skin. Tablets, sprays and gels are taken/applied daily and skin patches are usually changed twice weekly.
If you are prescribed HRT when you are still having periods, you will be given a type that still gives you monthly bleeds. If you have not had your period for at least one year you will be given a type of HRT that does not give you a bleed.
In some cases, HRT is required for vaginal symptoms alone (such as dryness, soreness or painful sex). In this case, you may require only topical treatment – a low dose oestrogen in the form of a pessary, gel, cream or a silicone ring (inserted into the vagina). The ring (called Estring in the UK) may be the best option for you if it is difficult or not possible for you to insert the pessaries or cream into your vagina yourself. Topical vaginal treatment can be taken in conjunction with systemic HRT (as above) or used alone. A relatively new vaginal treatment – a daily pessary containing dehydroepiandrosterone (DHEA) – has recently become available for vaginal symptoms and is licensed for the treatment of painful sex during menopause. In the last few years, a new non-hormonal treatment for vaginal symptoms, taken as a tablet by mouth, has also come onto the UK market.
Of course, you may be unable to take HRT for medical reasons (e.g., a hormone dependent cancer). In this case, there are alternative medications that may help, including certain types of anti-depressants such as fluoxetine or venlafaxine. These can improve symptoms such as hot flushes, even in women who are not depressed. Although most of these alternative medications have only been evaluated for their impact on vasomotor symptoms (i.e., flushes and sweats), some also have a positive impact on mood, well-being, pain and sleep.
Is HRT safe?
More up to date studies have shown numerous benefits of taking HRT and that any associated risks are very small.
For the vast majority of women, if started within ten years of menopause, below the age of 60, HRT has more benefits than risks and is generally safe and effective.
What are the benefits of taking HRT?
HRT also reduces your risk of osteoporosis, heart disease (if started within ten years of menopause), diabetes and colorectal (bowel) cancer (if taking combined HRT).
HRT is also very important for brain health in women who experience an early menopause and POI, and may reduce their risk of developing dementia later in life.
What are the risks of taking HRT?
Many women worry about the risk of developing breast cancer on HRT. This is a complex subject, as breast cancer is a complex disease. If you are taking certain forms of combined HRT (both oestrogen and a progestogen), then you may have a small increased risk of breast cancer if you take it for more than 5 years. However, the overall increase in risk is very small, and taking HRT does not appear to increase a woman’s risk of dying from breast cancer. For women who have had a hysterectomy and are on oestrogen-only HRT the increased risk of breast cancer is lower than it is with combined HRT.
A number of different factors are associated with a higher risk of developing breast cancer than that which comes from taking HRT; these include: being overweight, drinking 4+ units of alcohol (e.g., 2 medium sized glasses of wine) most days, smoking and doing little to no exercise. Therefore, it is important to put this into perspective if you feel you may benefit from HRT. Exercising for at least 2.5 hours per week is associated with a significantly reduced risk of breast cancer, so staying physically active is one of the most important things you can do (whether or not you choose, or are able, to take HRT).
Importantly, there is no increased risk of breast cancer in women who take HRT, compared with premenopausal women of the same age, under the age of 51.
For women who take a tablet form of HRT, there is a small increased risk of developing a blood clot. This risk is greater for women who are overweight, who smoke, who have had a clot in the past, or who have a medical history of diabetes or migraine. However, there is no increased risk of developing a blood clot if HRT is taken in the form of a gel, spray or patch (which means that women who do suffer with migraine, or have diabetes, for example, can take this form safely).
If HRT is started within ten years of menopause, below the age of 60, then there is no increased risk of heart disease; in fact, as mentioned above, there is evidence that HRT appears to reduce this risk. We used to think that if HRT is started after the age of 60 there may possibly be a very small increased risk; however, more recent research has demonstrated that, although there may be no cardiovascular benefit to starting HRT at this age, there is unlikely to be any harm.
What are the side effects of HRT?
The most common side effects are nausea (feeling sick), breast tenderness, mild headaches and leg cramps. These usually settle within the first month (and usually within a few days).
Some women experience some vaginal spotting or irregular bleeding when they first start HRT. This usually happens in the first 3-6 months of treatment as your body gets used to the hormones. If any unscheduled bleeding happens after this time it is very important that you see your doctor. Most of the time, all that will be required will be a change in medication. In some cases, you may be referred for an ultra-sound scan to check the thickness of the lining of your womb (again, this is rarely anything to worry about but may be important to rule out a more serious cause for your bleeding).
Are there any non-medical alternatives to HRT?
You may choose not to take HRT, or be unable to take it for other medical reasons.
There is some evidence that phyto-oestrogen supplements (e.g., soya and red clover) can improve menopausal symptoms. However, please note, these are not recommended if you have a history of hormone-dependent cancer, as there has not been enough evidence to evaluate their long-term safety. That said, dietary phyto-oestrogens (e.g., minimally processed soya foods) are recommended for all (allergies aside, of course) – regular intake of soya is associated with fewer menopausal symptoms and a reduced risk of breast cancer recurrence in breast cancer survivors.
Herbal preparations, e.g., black cohosh and sage, may also be helpful. However, if you choose to go down the herbal route it is important to understand that these may interact with other medications you may be taking. As such, always discuss this with your doctor or a pharmacist before starting a herbal medication.
If you buy herbal medicine over the counter, ensure that it has the THR registration (for quality standard and safety). You may wish to consult with a trained medical herbalist e.g., someone who is registered with The National Institute of Medical Herbalists. They will be able to advise you on all your options and will be aware of possible interactions between herbs and prescribed medications.
Cognitive-behavioural therapy (CBT) has been shown to be helpful for a number of menopausal symptoms including depressed mood, hot flushes and insomnia. Regular yoga practice has also been shown to improve both physical and emotional/psychological symptoms of menopause, and improve quality of life. The data is mixed regarding the benefit of acupuncture for menopausal symptoms, but some people find it helpful for associated headaches and joint/muscle aches.
Clinical Guidelines
Premenstrual Disorders (PMS/PMDD/PME)
Royal College of Obstetricians & Gynaecologists (RCOG): Management of Premenstrual Syndrome
IAPMD: Evidence Based Management of Premenstrual Disorders (PMDs)
RCGP Women’s Health Toolkit
Women’s Health Toolkit
This toolkit aims to provide those working in primary care with a one-stop resource for all their women’s health educational needs.
Useful Links
.
Menopause and POI
Menopause Care
Founded by Naomi Potter, Menopause Care is Britain’s largest team of British Menopause Society (BMS) registered doctors and healthcare professionals, offering both online and face-face-face consultations and support.
Women’s Health Concern
The patient arm of The British Menopause Society (BMS)
Menopause and Women’s Health in Later Life (RCOG)
Information hub for patients from The Royal College of Obstetricians & Gynaecologists
Ask Early Menopause
A website and app with information, personal stories, a dashboard and discussion forum for women with POI or early menopause.
The Daisy Network
Charity dedicated to providing information and support for patients with POI/premature menopause (below the age of 40)
The Surmeno Connection
An online resource and support group for women in surgical menopause
Menopause and Cancer
Menopause and Cancer is the a non-profit supporting cancer survivors through treatment-induced menopause.
Menopause Support
Menopause Support is a not for profit community interest company and the home of the national #MakeMenopauseMatter campaign, both founded by Diane Danzebrink.
Global Menopause Inclusion Collective
A collaboration of menopause peers interested in advancing equity and inclusion in the menopause movement
NHS HRT Prescription Prepayment Certificate
If you pay for NHS prescribed HRT medication 3 or more times in a 12 month period, an HRT PPC could say you money. Click on the link for further info and to buy an HRT PPC.
Premenstrual Disorders
National Association for Premenstrual Syndromes (NAPS)
UK charity working to support sufferers and raise awareness of Premenstrual Syndrome(s) – PMS/PMDD/PME
International Association for Premenstrual Disorders (IAPMD)
Not-for-profit organisation providing support and information for those affected by Premenstrual Dysphoric Disorder (PMDD) and Premenstrual Exacerbation (PME) of underlying disorders. US based, but with global links.
The Etiology of Premenstrual Dysphoric Disorder: 5 Interwoven Pieces
A good article summarising what is currently known about the likely causative and contributory factors relating to PMDD. Please note, this is written for health care professionals, using scientific/medical terminology.
Pelvic and Sexual Health
Squeezy App
An app that helps people improve their pelvic floor health with audio-visual guides, reminders, and progress tracking. Designed by NHS physiotherapists.
Obstetric and Gynaecological Physiotherapy (POGP UK)
Includes patient information on all aspects of pelvic health and a searchable directory of POGP physiotherapists.
Pelvic Pain Support Network
Providing support, information and advocacy for those living with pelvic pain
Vulval Pain Society
Charity dedicated to promoting and protecting the physical and mental health of sufferers of vulval pain through the provision of support, education and practical advice.
Vaginismus
Information and advice on vaginismus (NHS website)
CICS Recommended Sex & Relationship Therapists
Sex and relationship therapists recommended by the Contemporary Institute of Clinical Sexology (CICS) for help with sexual or relationship concerns.
Sexual Health & Pleasure Blog
Includes posts on low libido in menopause, sex after cancer, sex and lichen sclerosus, pudendal neuralgia, vaginal lubricants…and much more.
The surprising truth about desire everyone needs to know
A 15 minute TEDx talk on sexual desire by Dr Karen Gurney, a clinical psychologist specialising in the theory and practice of therapy around sexual wellbeing and function
Lifestyle Medicine
Live Well – NHS
NHS advice about healthy living, including eating a balanced diet, healthy weight, exercise, quitting smoking and drinking less alcohol.
Plant-based Health Professionals UK
Mission statement: “To educate health professionals, members of the public and policy makers on the benefits of whole-food plant-based nutrition in preventing and treating chronic disease”. Includes fact sheets and a directory of UK plant-based doctors.
Insight Timer
Free meditation app, including breathing exercises and Yoga Nidra
Yoga with Adriene
Free online yoga sessions ranging from 5 mins to 45 mins in length.
Jessica Valant – Pilates
Free online Pilates and body-weight workouts for everyone, including adaptations for a variety of different injuries and conditions.
Parkrun
Whether you walk, jog, run, volunteer or spectate, parkruns are free weekly community events all around the world.
Make Your Move
A series of short physical activity videos, created especially for people with long term health conditions, who may experience the common symptoms associated with these, such as pain, stiffness and fatigue.
Sleepio
A six-week clinically proven programme used to treat insomnia (NHS funding available in some areas).
Sleepstation
Sleep improvement and insomnia course, using CBTi principles (NHS funding available in some areas).
Reading Well
Reading Well supports you to understand and manage your health and wellbeing using helpful reading.
Thriving with Nature
WWF and the Mental Health Foundation have come together to produce a guide to help people thrive and for nature to thrive around them.
Nature and Mental Health
Tips from MIND for bringing nature into your everyday life to benefit both your mental health physical wellbeing.
Articles / In The Media
Surgical Menopause Questions and Answers
Updated July 2025
‘The menopause industry is thriving because women aren’t getting the care they need from the NHS’
Women’s Health, October 2024
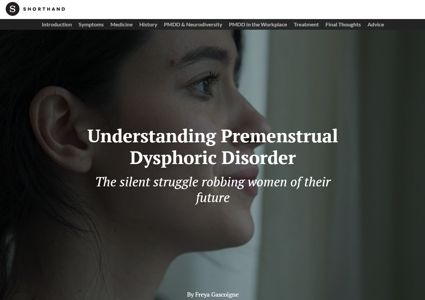
Understanding Premenstrual Dysphoric Disorder
Shorthand, June 2023
PMDD: Women call for more awareness of Premenstrual Dysphoric Disorder
BBC News, July 2020
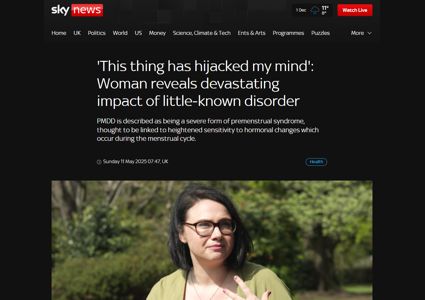
'My periods make me suicidal'
BBC News, July 2020
How It Feels To Go Through Early Menopause
Vogue, October 2019
Dr Hannah Short on being a plant-based GP
Originally published on ProVeg International (proveg.org), March 2019. Updated Sept 2020
ProVeg is going to Parliament! “Change can’t come soon enough”: Dr Hannah Short
Let’s talk menopause because we are failing 13 million women
The Guardian, April 2015
The H word
Platinum Magazine

#MakeMenopauseMatter
Photo from a visit to the Houses of Parliament to discuss the #MakeMenopauseMatter campaign.
Patient information leaflets
Your Guide to Menopause
I was a clinical reviewer on this one – it is free to download from this website, or paper copies can be ordered for a fee
The Thalidomide Trust: Menopause
Includes factsheets and vlogs on menopause, HRT, alternatives to HRT & lifestyle advice. Written primarily for beneficiaries of the Trust, but contains generic information useful for all.
Publication in peer reviewed journals
‘Unheard and undertreated’: Menopausal mental health (September editorial)
Post Reproductive Health
Editorial Chronic Conditions and Menopause
Post Reproductive Health
Signs of recovery . . . appropriate menopause care being made a priority?
Post Reproductive Health
The role of social media in menopausal healthcare
Post Reproductive Health
A Case of Subacute Thyroiditis Presenting with Oligomenorrhea
Gynecology & Obstetrics
Commissioning for menopause specialist services: A local perspective
Post Reproductive Health
Changing the change
Post Reproductive Health
Menopause and hormone replacement therapy
InnovAiT: Education and inspiration for general practice
Podcasts
Understanding My Body Through My Mind by Celia Manuel
PMDD Unmasked: The Battle No One Sees
In a Nutshell: The Plant-Based Health Professionals UK Podcast
Periods, PMS, and PMDD: how can diet and lifestyle help, with Dr Hannah Short
The Premature Menocast
Episode 9: Interview with POI Author Dr Hannah Short
Hysterical
The Complete Guide to POI with Dr. Hannah Short & Dr. Mandy Leonhardt
MENOMORPHOSIS
#63 Endometriosis, PMS And Premature Ovarian Insufficiency With Dr Hannah Short
Blue Mumdays
The One About Hormones – POI, PMDD, Endometriosis + PME: Dr HANNAH SHORT
Dr Streicher's Inside Information: THE Menopause Podcast
Ep 56: Too Young for Menopause?
With All Due Respect! by Amanda Thebe
Dealing with POI or Early Menopause – with Dr Hannah Short & Dr Mandy Leonhardt
WomenKind Collective
POI (premature Ovarian Insufficiency) & Early Menopause with Dr Mandy Leonhardt & Dr Hannah Short
The Best of Health
3.1 Dr Mandy Leonhardt & Dr Hannah Short – Premature Ovarian Insufficiency and Early Menopause
The Menopause and Cancer Podcast
Ep 9: Early Menopause through Surgery with Dr Hannah Short
The Sexual Wellness Sessions
Understanding Induced Menopause With Dr Liz O’Riordan & Dr Hannah Short
The Dr Louise Newson Podcast
PMS and the Menopause – Dr Hannah Short and Dr Louise Newson
The Doctor's Kitchen Podcast
#63: Eating for The Menopause with Dr Hannah Short
Infinite Potential Podcast
Ep18: Understanding Menopause with Dr Hannah Short
Liz Earle Wellbeing Podcast
PMS and PMDD with Dr Hannah Short
BBC Woman's Hour
Talking to your kids about race, HRT shortages, and the demise of the bonkbuster novel
Fit n' Chips Chats
Episode 52 Dr Hannah Short – Menopause + PMS Specialist GP
The Ditch the Diet Podcast
How to Manage the Menopause with Dr Hannah Short
Liz Earle Wellbeing Podcast
Surgical menopause and hormonal health with Dr Hannah Short
Videos and webinars
General
The Holistic Management of Premenstrual Disorders: A Lifestyle Medicine Approach – Plant-Based Health Professionals UK
Premature Ovarian Insufficiency (POI) and Early Menopause: A Lifestyle Medicine Approach – Plant-Based Health Professionals UK
Dr Hannah Short and Dr Mandy Leonhardt talk about premature menopause with Diane Danzebrink
Doctor’s Kitchen
Menopause – an information webinar
Women’s voices at the RCOG